General Health Info
Medical / Health Information
Seasonal Flu Vaccine
What is influenza (flu)?
Influenza is a highly infectious acute respiratory illness caused by the influenza virus. Influenza affects people of all ages. Outbreaks of influenza occur almost every year, usually in winter. This is why it is also known as seasonal flu.
Pregnant ladies can be given the flu vaccine at any stage of pregnancy.
How serious is flu?
Flu is often self limiting with most people recovering in 2-7 days. However, flu can be severe and can cause serious illness and death, especially in the very young and in the elderly. Serious respiratory complications can develop, including pneumonia and bronchitis, to which older people and those with certain chronic medical conditions are particularly susceptible.
Pregnant women have also been found to be at increased risk of the complications of flu. Some people may need hospital treatment and a number of mainly older people die from influenza each winter.
How do people catch flu?
Flu is a highly infectious illness. A person carrying the virus can spread the illness by coughing or sneezing. A person can spread the virus from 1-2 days before they develop symptoms and for up to a week after symptoms develop.

What are the symptoms of Flu?
Flu symptoms hit you suddenly and severely. Symptoms of flu include:
- sudden fever
- chills
- headache
- myalgia (muscle pain)
- sore throat
- non-productive dry cough
Is it seasonal flu or the common cold?
It can be difficult at times to tell between the common cold and flu. A cold is a much less severe illness than flu. The flu symptoms come on suddenly with fevers and muscle aches. A cold usually starts gradually with symptoms of a sore throat and a blocked or runny nose.
Table of Symptoms
The following table provides information on how to distinguish between seasonal flu and cold symptoms.
| Symptoms | Seasonal flu | Cold |
|---|---|---|
| To make an appointment, contact us on (01) 873 59 59. | ||
| Fever | High fever lasts 3-4 days | Rare |
| Headache | Prominent | Rare |
| General Aches, Pains | Usual, often severe | Slight |
| Fatigue, Weakness | Can last up to 2-3 weeks | Quite mild |
| Extreme Exhaustion | Early and prominent | Never |
| Stuffy Nose | Sometimes | Common |
| Sneezing | Sometimes | Usual |
| Sore Throat | Sometimes | Common |
| Chest Discomfort, Cough | Common; can become severe | Mild to moderate; hacking cough |
Who is most at risk from flu?
Anyone can get the flu but it is more severe in people aged 65 years and over and anyone with a chronic medical condition. Chronic medical conditions include chronic heart conditions, chronic respiratory disease, diabetes mellitus and immunosuppression due to disease or treatment. Pregnant women have also been found to be at increased risk of the complications of flu. These groups of people are targeted for influenza vaccination.
How can flu be prevented?
Flu can be prevented by vaccination. Flu vaccine is a safe, effective way to help prevent flu infection, avoiding hospitalisation, reducing flu related deaths and illnesses.
Seasonal Flu Vaccine Price
| Service | Price | Notes |
|---|---|---|
| All consultations incur a charge. If you have had blood tests taken you will be asked to make a review appointment to discuss the results with your GP. | ||
| To make an appointment, contact us on (01) 873 59 59. | ||
| Flu Vaccine | €25 | Can be given at any stage of pregnancy. Whooping cough also available for pregnant ladies of this clinic €25 |
What is the seasonal (annual) flu vaccine?
Each year the seasonal (annual) flu vaccine contains three common influenza virus strains. The flu virus changes each year this is why a new flu vaccine has to be given each year. This year’s flu vaccine contains the Swine Flu strain.
What strains are in this year’s seasonal flu vaccine?
This year’s seasonal flu vaccine contains 3 strains of flu viruses as recommended by the World Health Organization (WHO) and has been manufactured in a similar way to previous seasonal vaccine. The three strains are:
- A/California/7/2009 (H1N1)-like virus (the pandemic H1N1 2009 virus)
- an A/Perth/16/2009 (H3N2)-like virus
- a B/Brisbane/60/2008-like virus
Who should be vaccinated?
Vaccination is strongly recommended for:
- persons 65 and over
- those with a long-term medical condition such as diabetes, heart or lung disease
- people whose immune system is impaired due to disease or treatment
- healthcare workers
- residents of nursing homes and other long stay institutions
- persons with a body mass index (BMI) over 40
- pregnant women. (can be given at any stage of pregnancy)
- carers
- people with regular close contact with poultry, water fowl or pigs
How does seasonal flu vaccine work?
How safe is flu vaccine?
Will the flu vaccine give me the flu?
When should I get vaccinated?
What should I expect after vaccination?
How long does it take the vaccine to work?
Who should NOT get seasonal flu vaccine?
What about people with egg allergy?
When should vaccination be postponed?
What is Swine Flu?
Why is the Swine Flu strain in this year’s vaccine?
Is it safe to give seasonal vaccine to people who received Swine Flu vaccine in 2009-2010?
What about Avian Flu?
Avian or bird flu due to the H5N1 virus has spread rapidly throughout poultry flocks in Asia and more recently to Eastern Europe. It is proving difficult to eradicate in birds.
Humans are rarely affected with avian/bird flu and this has mainly happened through close contact with live infected birds or their faeces.
Does the seasonal flu vaccine protect against Avian Flu?
Remember
If you are over 65 or have a long term medical condition you should also ask your doctor about the pneumococcal vaccine which protects against pneumonia, if you have not previously received it.
Keep well this winter
- Eat well: eat at least one hot meal a day.
- Keep warm: wear several layers when outside and keep at least one room heated during the day.
- Keep active.
- Get vaccinated.
Diabetes Explained
Carbohydrates
Fats
Protein
Glucose uptake
Glucose is very important because the body needs sugar at all times to keep the cells alive and to provide energy for the brain. Before it can be used as energy glucose must enter cells such as the muscle and brain cells where it is needed for movement and mental activity, the liver where it is stored as a quick source of energy and the fat cells where any excess food is converted to fat and goes into long-term storage. Glucose cannot just flow into these cells from the blood, it must move through channels on the cell surface. Insulin binding to the insulin receptor on the cell surface allows these channels to open and glucose can enter the cell.
Type 1 Diabetes
Normally insulin is produced by the beta cells in the pancreas. In Type 1 diabetes the beta cells have been destroyed and therefore insulin is not produced. Only 10% of the population with diabetes have type 1 diabetes. Although there is a genetic predisposition to Type 1 diabetes it is not usually inherited and there is a very low risk of diabetes for the child of a person with diabetes. People with type 1 diabetes are seldom overweight. Antibodies to insulin-producing cells are found in newly diagnosed Type 1 diabetic patients and it is thought a virus infection suffered by a person with susceptible genes may be a trigger for diabetes. However, this is only one theory and recent research suggests that there may be other factors involved in the development of Type 1 diabetes
At first, sufficient insulin is produced as the pancreas is deteriorating and blood glucose remains normal until almost all the beta cells have been destroyed. A person who is developing Type 1 diabetes only becomes sick when almost all the beta cells have been destroyed and they have almost no insulin. The beta cells do not usually recover once diabetes has developed although recent research has shown that it may be possible in the future to provide the conditions necessary for the beta cells to recover but this will be a long-term project. New research suggests that it may soon be possible at least to prevent the complete destruction of the beta cells but treatment must be given at the early onset of the condition.
Type 1 diabetic patients must be treated with insulin and the aim of treatment is to keep their blood sugar as close to normal as possible
Type 2 Diabetes
Type 2 diabetes affects 10% of the population over 50 and is increasing at an alarming rate. 90% of people with diabetes have Type 2 diabetes. Factors which make people susceptible to Type 2 diabetes are:
- Being overweight
- Being overweight
- Having a family history of diabetes
- Age over 40
- Have had diabetes in pregnancy
- Had a large baby
- Lack of exercise
The older people get the more likely they are to develop diabetes. Type 2 diabetes comes on slowly and it is estimated that on average diabetes has been present for 7 years prior to diagnosis. It is very important that diabetes is diagnosed so that it can be treated and the complications of diabetes can be avoided. High blood sugars cause heart disease, kidney disease, damage to the back of the eye and foot ulcers.
People who have Type 2 diabetes have a defect in the beta cells of the pancreas causing them to produce insufficient insulin. These patients need pills to stimulate the beta cell to produce more insulin and if that does not work they need to be given insulin. People who are overweight and develop Type 2 diabetes may also be insulin resistant. That means that the patient’s cells are producing plenty of insulin, maybe much more than normal, but the patient’s muscle, liver and fat cells are resistant to the action of insulin and they need much more insulin to enable them to utilise glucose. Insulin resistance is associated with being overweight, having a poor diet and taking little exercise. Treatment consists of a weight-reducing diet and pills to make the cells more sensitive to the action of insulin. However, they also have a defect in insulin production and may need to take insulin eventually.
Measuring blood sugar levels
Blood sugar should be monitored regularly by both Type 1 diabetic patients and usually by Type 2 diabetic patients. Patients on insulin are usually asked to measure their blood sugar 4 times a day so that adjustment of insulin can be made at regular intervals. Type 2 diabetic patients usually measure their blood sugar only once or twice a day or less often if they are very stable.
Blood sugar is easily measured using a glucose meter. These are very small, light weight and simple to use. It only takes a very small drop of blood from a finger prick. A spring-loaded pricking device which is almost painless, is used to take the blood which is applied to a strip in the glucose meter and the glucose reading appears in 5-10 seconds. Fasting blood sugar should be between 4 and 6mmol/l
Continuous glucose monitoring
Continuous Glucose Monitoring System is a device which is implanted under the skin and takes a blood glucose measurement every 5 minutes throughout the day and night, for up to 3 days. It may either be used like a watch with a read-out and may be downloaded later to a computer. This way the patient and their physician can see exactly what is happening to the blood glucose levels round the clock. The sensor is inserted under the skin and is connected to a small pager-sized monitor. An electronic signal proportional to the blood glucose level is transmitted to the monitor.
Dietary Advice
A normal healthy diet is advised for people with diabetes. A healthy diet is one that contains a high percentage of vegetables and fruit, a moderate amount of protein (meat, fish, eggs, cottage cheese), a low amount of fat (cheese, meat, sauces) and in particular a low animal fat diet. People who are overweight need to reduce the calorie content of their diet by eating less food and drinking less!
Loosing weight is difficult. Many people are surprised by the number of calories contained in fruit and vegetables. Refined sugar is absorbed very quickly and is best avoided except at the end of the meal when absorption will be delayed because of the other food in the stomach. Remember refined sugar is high in calories and low in appetite suppression! Cakes and sweets will increase blood sugar rapidly.
General Cooking Tips
- Do not fry. Instead grill, bake, poach, steam, microwave or boil foods.
- Use low fat dairy products, such as skimmed or semi-skimmed milk.
- Use fats or oils which are high in monounsaturates (olive oil).
- Try to use brown rice or pasta in place of white rice as it contains more fibre. If you choose a lower fibre variety of rice or pasta, serve it with higher fibre foods like extra vegetables.
- Choose high fibre rather than low fibre carbohydrate foods (e.g. wholemeal bread). Use low fat cheddars or cottage cheese.
Rich sauces such as thick gravies, mayonnaise and salad cream should be avoided, if you need to lose weight or your cholesterol is high. Use light mayonnaise or low-calorie salad creams instead. Consider using natural or diet yoghurt instead of cream or light cream.
A high salt diet may increase blood pressure. Avoid processed meats and foods. Sausages, hamburgers, meat pies, crisps, chips and oven chips have high-fat content and a lot of salt (People with high blood pressure especially should reduce their salt intake).
A moderate amount of protein (e.g. meat, poultry, fish, cheese) is recommended.
Carbohydrate advice for people with diabetes
There are three types of carbohydrates, each of which have different effects on blood glucose levels:
- Refined sugars (sucrose, glucose or fructose) increase blood glucose levels very rapidly and should be used urgently to correct ‘hypo’ attacks.
- Starchy foods with a high fibre content rather than low fibre starches are recommended. This delays absorption and improves control of diabetes.
- Low fibre starches are white bread, rice, potatoes, pastas and breakfast cereals such as cornflakes. High fibre starches: wholemeal bread, brown rice, brown pasta, wholegrain cereals such as bran cereals and porridge.
Diabetic products
Foods labelled ‘suitable’ for people with diabetes are usually not suitable due to their high-fat content. Non-calorie sweeteners may be used freely. Products sweetened with artificial sweeteners can be taken freely.
Remember, if you are overweight and have been advised to lose weight you must reduce your food.
Alcohol
Alcohol may be included as part of a healthy diet but remember alcohol stimulates insulin secretion in people who still have some beta cells and may cause hypoglycaemia in type 2 patients.
Never drink on an empty stomach and do not substitute alcohol for food. It may be necessary to eat with or shortly after alcoholic drinks. Test your blood sugar after alcohol ingestion to ensure the maintenance of good control. Avoid sweet wines, cider and liqueurs. If you dilute spirits use soda water and sugar-free mixers. If you are overweight, keep your alcohol intake low since alcohol is high in calories.
Remember to inform your friends/colleagues that you have diabetes and take insulin. They should be instructed in the symptoms of hypos and if they see you behaving in a strange manner they must insist that you either do your blood sugar to make sure it is normal or else insist that you take sugar. You may not recognise the symptoms of hypo when you have taken alcohol and your friends may just think you are drunk. That may be a very dangerous mistake to make.
Living and Lifestyle
Regular exercise keeps you fit, controls your weight, allows insulin to work better and reduces the risk of heart attack and stroke. Regular exercise is important for a long and healthy life. Virtually all sports are open to people with diabetes and indeed many world class athletes have diabetes. Depending on the type of exercise, you may need to lower your insulin dose and increase your food to avoid low blood sugar levels (hypos). Vigorous and prolonged daytime exercise may cause hypoglycaemia during the night, and extra carbohydrate may be necessary at bedtime.
Holidays and Travel
Diabetes does not prevent you from experiencing new places or cultures. For example, a team sponsored by the Diabetes Federation of Ireland successfully climbed Kilimanjaro, the highest mountain in Africa.
Before travelling it is advisable to:
- Contact your family doctor or clinic to get the necessary vaccinations.
- Bring a letter from the Clinic to explain that you need to carry syringes/needles etc in the cabin.
- Arrange adequate medical insurance (The diabetes Federation of Ireland has special offers).
- Carry a diabetes identity card or engraved discs/bracelets wherever you are going.
- Discuss managing sickness and diarrhoea with the Clinic beforehand. As a precaution, drink only bottled water, avoid salads in hot and underdeveloped countries and consider hygiene levels in restaurants.
- Keep insulin cool (e.g. in a thermos flask) and wrap the pens, cartridges, vials etc in cotton wool, tissue or paper to prevent breakages.
- Carry insulin, pens, syringes and other equipment in hand luggage. When travelling by air, insulin should not be stored in the main baggage area as it may freeze, making it less effective.
To maintain good control of your diabetes, be extra vigilant with blood-glucose testing to monitor the changes of routine and food.
Always carry glucose sweets or a fast-acting carbohydrate.
Find out what types of insulin are available abroad in case of emergencies. If you are taken ill on holiday, never stop your insulin even if you cannot take food or drink. Usually, illness requires increased doses of insulin. Test blood sugar every hour and take quick-acting insulin to keep blood sugar levels normal. Make sure you know what to do if you’re suffering from an acute illness.
Cholesterol and Heart Disease
One of the best ways to prevent heart disease is to keep your cholesterol at a healthy level.
Heart disease can be inherited, so if someone in your family has the disease, it is likely you may also get it. If you already have heart disease, or there is a history of heart disease in your family, making small healthy changes now can make a difference to your life today and tomorrow.
Why is cholesterol important?
Having high cholesterol levels in your blood is one of the risk factors which increases your chances of getting heart disease.
What is cholesterol?
Cholesterol is a type of fat found in your blood. You need a certain amount of cholesterol for all your body cells and to produce important hormones. However, if there is too much cholesterol in your blood, it sticks to the inner lining of your artery or blood vessels to form atheroma. As a result of this build-up on the artery walls, your arteries become narrowed. This process is called hardening of the arteries or atherosclerosis.
If an artery supplying the heart muscle becomes blocked completely, the heart muscle becomes damaged. This is known as a heart attack. If an artery to the brain is completely blocked, it damages the brain. This is called a stroke.
Where does cholesterol come from?
Cholesterol is made in the body mainly by the liver. This is often called blood cholesterol. The body can produce all the cholesterol it needs to carry out its many functions and can usually maintain a healthy level of blood cholesterol. However, sometimes the balance goes wrong and there is an increase in blood cholesterol. This may result from inherited problems or from eating too much saturated (animal) fat. Some foods such as eggs, liver and shellfish contain cholesterol. However, the amount of cholesterol in these foods does not greatly affect the amount of cholesterol in your blood. You can eat foods that contain cholesterol in moderation as part of a healthy varied diet.
Confused about cholesterol?
The relationship between cholesterol and heart disease is very complicated but it helps to look at how cholesterol is carried around in the bloodstream. There are two main types of cholesterol:
– HDL cholesterol (high-density lipoprotein)
– LDL cholesterol (low-density lipoprotein)
HDL cholesterol is called good cholesterol or healthy cholesterol because it mops up cholesterol left behind in your arteries and carries it to the liver where it is broken down and passed out of the body. Regular physical activity and exercise can help increase your HDL level. High levels of HDL cholesterol can protect you against getting heart disease.
LDL cholesterol (low-density lipoprotein) from the liver through the arteries to other parts of the body. LDL is called bad cholesterol because it sticks to the walls in your arteries – making them narrow. This reduces the blood supply to your heart or brain. Eating too many foods high in saturated fat can raise your LDL cholesterol. High levels of LDL cholesterol increase your risk of heart disease.

Confused about fats?
Fats in food are a mixture of saturated and unsaturated fats. Choose sunflower, olive or Polyunsaturated and monounsaturated fats are unsaturated fats that can help lower the amount of LDL cholesterol in your blood and reduce your chances of getting heart disease.
Polyunsaturated and monounsaturated fats are found in most pure vegetable oils like sunflower, olive and rapeseed oils. You also find them in the spreads and margarine made from these oils, as well as in many types of nuts. You also find polyunsaturated fats in oily fish such as sardines, mackerel, trout and salmon (tinned or fresh).
Saturated fats can raise your LDL cholesterol and increase your chances of getting heart disease. You find saturated fats in foods like butter, hard margarine, lard, cream, cheese, fatty meat, cakes, biscuits and chocolates.
Check the food labels on processed and ready-made meals for the amount of saturated fats.
Is your cholesterol level too high?
If you need to change any aspects of your cholesterol or triglyceride levels, your doctor will advise you on changes in lifestyle and may recommend medication. If you are prescribed medication, it is important that you follow the instructions carefully.
How can I lower my cholesterol?
- Eat more fruit and vegetables.
- Eat more wholegrain cereals and breads, plenty of jacket potatoes and rice and pasta.
- Choose lean meats. Trim fat off meat and skin off chicken.
- Drain oil from cooked dishes containing minced meat.
- Choose low-fat dairy products.
- Choose low-fat spreads made from sunflower or olive oil.
- Use low-fat healthy ways of cooking, like grilling or oven-baking, instead of frying.
Cholesterol-lowering foods
What if I have low HDL?
You can increase the healthy HDL levels by:
- being more active
- reducing your weight; and
- if you smoke, by stopping smoking
Your doctor may also prescribe medication to raise your HDL levels.
What are triglycerides and how do they affect my heart?
Could I have high triglycerides?
- are overweight
- drink too much alcohol
- eat lots of sugary foods; or
- are not very active
Ask your doctor to check your triglyceride levels.
Check out the other risk factors for heart disease High blood cholesterol is not the only risk factor for heart disease. Other risk factors are:
- smoking
- high blood pressure
- being overweight
- diabetes
- not being active
- stress that you cannot control
- your family history
- your age
If you have high cholesterol plus any of these risk factors, it is important that you talk to your doctor.
For a healthy cholesterol and a happy heart:
- eat more fruit and vegetables and wholegrain foods
- eat less fatty foods
- eat oily fish twice a week
- if you smoke, try to stop
- be a healthy weight
- be more physically active every day
- drink less alcohol
- learn to relax – take time out for yourself
- have a regular blood pressure and cholesterol check with your doctor.
Bladder Problems
What are Bladder Problems?
A bladder problem is a medical condition that prevents you from being able to control when you pass urine, characterised by one or more of the following symptoms:
- A frequent need to pass urine (8 times or more during a 24-hour period)
- A strong, sudden urge to pass urine
- Waking up to pass urine (2 or more times a night)
- Wetting yourself (small or large amounts)
If you live with bladder problems, you are not alone. Millions of men and women of all ages also share these problems.
There are 3 major type of bladder problems. Each has a different cause and exhibits different symptoms.
Overactive Bladder
Overactive bladder (OAB) is a treatable medical condition that affects approximately 300,000*1sup> people in Ireland. This condition is not normal at any age.
Symptoms
- Frequency – having to go to the toilet more than 8 times over 24 hours. If you wake up to go to the toilet more than once during the night you may have a condition called nocturia i.e. frequency at night.
- Urgency – strong, sudden need to go to the toilet that necessitates rushing to the toilet.
- Urge – this is an overwhelming urgency to urinate but not having enough time to get to the toilet. This results in wetting accidents.
If you answer yes to any of the questions below you should discuss your symptoms with your local GP or nurse, so they can ensure you get the treatment you need.
Cause
Overactive bladder occurs when a large muscle in the bladder known as the detrusor is too active. Instead of staying at rest as urine fills the bladder, the detrusor contracts while the bladder is filling with urine, usually more often than normal and at inappropriate times. This causes a person to feel a sudden and sometimes overwhelming urge to urinate even when the bladder is not full.
Although in many cases the reason for this contraction is unclear, for some people it may be due to a problem with the nerve signals that run from the brain to the bladder.
Some men with the symptoms of overactive bladder have an enlarged prostate rather than an overactive bladder. (However, it is also possible to have both an enlarged prostate and an overactive bladder). An enlarged prostate is not a bladder-related problem. A doctor can tell you whether your symptoms are due to an overactive bladder, an enlarged prostate, or both conditions.
Stress Incontinence
Stress incontinence refers to physical stress.
Stress incontinence Symptoms
- Leaking urine when coughing, sneezing, lifting, dancing, walking down the stairs, playing sport etc.
If you answer yes to any of the questions below you should discuss your symptoms with your local GP or nurse, so they can ensure you get the treatment you need.
Question 1: Do you experience a loss of urine when you are doing physical activities, such as lifting heavy objects or exercising?
Question 2: Do you sometimes have a slight loss of urine when you sneeze, cough, or laugh?
Causes of stress incontinence
The support muscles around your urethra, which is the outlet passage from the bladder, keeps the urine in your bladder from escaping. When these muscles become weak, even the small amount of stress created by everyday activities may cause a small amount of urine to pass.
In women, stress incontinence often occurs after pregnancy or menopause. In recent mothers, this is because muscles have been stretched and in postmenopausal females because of a lack of oestrogen. In men stress incontinence can occur after prostate surgery.
Mixed Incontinence
It is not uncommon for someone to have both the symptoms of an overactive bladder and stress incontinence.
Mixed incontinence symptoms:
- Frequency – having to go to the toilet more than 8 times over 24 hours.
- Urgency – strong, sudden need to go to the toilet which necessitates rushing to the toilet.
- Urge – this is an overwhelming urgency to urinate but not having enough time to get to the toilet. This results in wetting accidents.
- Leaking urine when coughing, sneezing, lifting, dancing, walking down the stairs, playing sport etc
Enuresis
Enuresis Symptoms
Wetting the bed at night (this is called nocturnal enuresis).
These tools can help you discuss your symptoms with your local GP or nurse, so they can ensure you get the treatment you need:
Causes of enuresis
Each individual is different and the causes are varied, however, some of the usual causes are:
- Urinary tract infection (UTI): any sign of blood, pain of difficulty in passing urine may indicate an infection. You should consult your local doctor.
- Alcohol, tea, coffee, fizzy drinks: drinking large amounts of these fluids prior to bedtime can irritate the bladder and cause bed wetting.
- Overactive bladder: there may be an interruption in the signals between the brain and the bladder. You may or may not be aware you want to pass urine but cannot wait until you reach the toilet.
- Stress and anxiety
- Stressful life events can contribute to bed wetting
- Small bladder capacity
- Family history
Urinary Tract Infection (UTI)
Urinary tract infections are perhaps the most common form of condition to be confused as an overactive bladder control problem. Occurring mostly in women but in some men, the term UTI refers to a variety of conditions including Cystitis (infection of the bladder), pyelonephritis (infection of the kidney), and urethritis (infection of the urethra).
UTIs are caused by bacteria (E.Coli) attaching itself to the walls of the bladder and growing. If this bacteria remains in the bladder and is not flushed out properly when you urinate infection can occur.
Symptoms
Symptoms are quickly noticeable (unlike overactive bladder):
- Frequent need to pass urine just as if you had the symptoms of an overactive bladder.
- Painful burning sensation when passing urine, and often only a small amount of urine is passed.
- Cloudy urine, lower back or abdominal pain, and blood in the urine.
Prostate Problems
Symptoms
- A weak and interrupted flow of urine.
- The need to urinate frequently during both the day and night.
- The need to urinate frequently during both the day and night.
- A burning sensation when urinating.
- A constant feeling that the bladder is not empty even after urination.
- Difficulty in beginning to urinate even when the bladder feels full.
- An urgent need to urinate straight away.
- Difficulty in urinating at all.
Bladder Stones
Bladder stones may come from the kidneys but most of the time they happen in the bladder. They can block the flow of urine in the urethra from the bladder to the outside.
Symptoms
- Pain when urinating
- Blood in the urine towards the end of urination
- Inability to urinate
If you think that you suffer from any of the above symptoms, discuss it with your doctor, because they can become serious if not taken care of immediately.
Quality of Life
Do you believe your overactive bladder control problem isn’t a major problem in your life? After all it is not a life-threatening condition, and you may be used to the way you have adapted your life around the symptoms. However, you should know that bladder control problems can be easily treated and are not normal at any age.
Here are just some of the ways a bladder control problem can interrupt and limit everyday life:
- Disturbed sleep and loss of daytime productivity due to waking up to go to the bathroom 2 or more times during the night.
- Withdrawal from sexual intimacy to avoid the anxiety and embarrassment caused by urine leakage during lovemaking.
- Lower-quality work due to frequent trips to the bathroom, the need to repeatedly leave meetings, and inability to concentrate.
- Lack of exercise caused by fear of being too far away from a bathroom.
- Habitual creation of “maps” of toilet locations, planning activities such as travelling and shopping based on knowing where toilets can be easily reached.
- Declining social invitations from friends and family because of the embarrassment of having to visit the bathroom regularly or the fear of having a wetting accident.
- Sitting in the aisles in public transportation, places of worship, the theatre, or at movies to be able to leave quickly to find a bathroom.
- Carrying a spare set of clothing in case of a wetting accident.
- Wearing dark and baggy clothing to disguise disposable pads or the signs of a wetting accident.
- Carrying a bottle in the car in case of the need to urinate while travelling long distances between petrol stations.
You may be able to think of more ways that your bladder control problem has changed your behaviour and maybe even affected the way you view yourself. The Facts and Figures section uncovers further evidence of the number of people with similar problems and how their lives are similarly affected.
Support For You
Although this Web site is no substitute for direct contact with your local doctor or nurse, the Support section can help you prepare for a visit to your local surgery.
These tools can help you discuss your symptoms with your doctor, so they can ensure you get the treatment you need.
How does your Bladder work?
The Urinary System
Your urinary system consists of two kidneys, two ureters, one bladder and one urethra. Most people have two kidneys but you can function healthily with one.
Urine Flow and Control
Step 1: Storing urine
Every time you eat and drink, your body absorbs liquids. The kidneys filter out waste products from the blood and make urine. Urine flows downward from the kidneys to the bladder through a pair of tubes called ureters.
The bladder is a balloon-like organ that changes shape according to the amount of urine it contains. It looks like a deflated balloon when it is empty and then becomes somewhat pear-shaped when the amount of urine inside increases.
Step 2: Releasing urine
Urine leaves the bladder and exits the body through a tube called the urethra.
The process of emptying the bladder – urination – is sometimes also called “voiding”. Urination is controlled by muscles, called sphincters, which surround the urethra. The sphincters keep the urethra closed by squeezing like tight rubber bands.
Pelvic floor muscles under the bladder also help keep the urethra closed. Urine stays inside the body when the sphincter and pelvic floor muscles are tight. When the bladder is full, nerves in your bladder signal the brain. That’s when you get the urge to go to the bathroom.
Once you reach a toilet, your brain sends a message to the large bladder muscle – called the detrusor – to contract so that it squeezes urine out of the bladder. At the same time, the brain tells the sphincter and pelvic floor muscles to relax and let the urine through. When you are finished urinating, the sphincters once again contract, and the bladder muscles stops squeezing and relaxes.
Knowing how a healthy bladder works will help you understand what happens when bladder control is a problem.
Irritable Bowel Syndrome
It is not the same as inflammatory bowel disease (IBD), which includes Crohn’s disease and ulcerative colitis.
Causes, incidence, and risk factors
There are many possible causes of IBS. For example, there may be a problem with muscles in the intestine, or the intestine may be more sensitive to stretching or movement. There is no problem with the structure of the intestine.
It is not clear why patients develop IBS, but in some instances, it occurs after an intestinal infection. This is called postinfectious IBS. There may also be other triggers.
Stress can worsen IBS. The colon is connected to the brain through the nerves of the autonomic nervous system. These nerves become more active during times of stress and can cause the intestines to squeeze or contract more. People with IBS may have a colon that is over-responsive to these nerves.
IBS can occur at any age, but it often begins in adolescence or early adulthood. It is more common in women. About 1 in 6 people in the U.S.have symptoms of IBS. It is the most common intestinal complaint for which patients are referred to a gastroenterologist.
Symptoms
Symptoms range from mild to severe. Most people have mild symptoms. Symptoms vary from person to person.
Abdominal pain, fullness, gas, and bloating that have been present for at least 6 months are the main symptoms of IBS. The pain and other symptoms will often:
- Occur after meals
- Come and go
- Be reduced or go away after a bowel movement
People with IBS may switch between constipation and diarrhea, or mostly have one or the other.
- People with diarrhea will have frequent, loose, watery stools. They will often have an urgent need to have a bowel movement, which is difficult to control.
- Those with constipation will have difficulty passing stool, as well as less frequent bowel movements. They will often need to strain and will feel cramping with a bowel movement. Often, they do not eliminate any stool, or only a small amount.
For some people, the symptoms may get worse for a few weeks or a month and then decrease for a while. For other people, symptoms are present most of the time and may even slowly increase.
People with IBS may also lose their appetite.
Signs and tests
Most of the time, your doctor can diagnose IBS based on your symptoms, with few or no tests. Eating a lactose-free diet for 2 weeks may help the doctor evaluate for a possible lactase deficiency.
There is no test to diagnose IBS, but tests may be done to rule out other problems:
- Blood tests to see if you have a low blood count (anemia)
- Stool cultures to rule out an infection
Some patients will have sigmoidoscopy or colonoscopy. During these tests, a hollow tube is inserted through the anus. The doctor can see through this tube. You may need these tests if:
- Symptoms began later in life (over age 50)
- You have symptoms such as weight loss or bloody stools
- You have abnormal blood tests (such as a low blood count)
Other disorders that can cause similar symptoms include:
- Celiac disease
- Colon cancer(although cancer rarely causes typical IBS symptoms, unless symptoms such as weight loss, blood in the stools or abnormal blood tests are present)
- Crohn’s diseaseor ulcerative colitis
Treatment
The goal of treatment is to relieve symptoms.
Lifestyle changes can be helpful in some cases of IBS. For example, regular exercise and improved sleep habits may reduce anxiety and help relieve bowel symptoms.
Dietary changes can be helpful. However, no specific diet can be recommended for IBS in general, because the condition differs from one person to another. The following changes may help:
- Avoid foods and drinks that stimulate the intestines (such as caffeine, tea, or colas)
- Avoid large meals
- Avoid wheat, rye, barley, chocolate, milk products, and alcohol
- Increase dietary fiber
Talk with your doctor before taking over-the-counter medications.
- Fiber supplements can make symptoms worse
- Laxatives taken for constipation can become habit forming
Counselling may help in cases of severe anxiety or depression.
Expectations (prognosis)
Irritable bowel syndrome may be a lifelong condition. For some people, symptoms are disabling and reduce the ability to work, travel, and attend social events.
Symptoms can often be improved or relieved through treatment.
IBS does not cause permanent harm to the intestines, and it does not lead to a serious disease, such as cancer.
Calling your health care provider
Call your doctor if you have symptoms of irritable bowel syndrome or if you notice a persistent change in your bowel habits.
What is Asthma?
Children with asthma have airways that are red and sensitive i.e. “inflamed”. They are easily irritated when they are exposed to asthma “triggers” e.g. the common cold. Symptoms include cough, wheeze, shortness of breath and chest tightness. Some or all of these symptoms may be present in any child. Asthma varies in severity. Some children can be almost symptom-free with only an occasional cough or wheeze while others can be very symptomatic.
What does asthma feel like?
Quotes from children with asthma. “It feels like someone is standing on my chest”, “It feels like I am being squashed”.
What are “asthma triggers”?
Asthma triggers can be anything that irritates the airways and “trigger the onset of asthma symptoms” (cough, wheeze, shortness of breath). Common triggers include the common cold, chest infections, house dust mite, exercise, cigarette smoke, animal dander and stress. Each child has different triggers. Identification and avoidance of triggers are important for each child.
What happens during an asthma attack?
During an asthma attack children may cough, wheeze, have difficulty breathing or be short of breath. Symptoms occur because the lining of the airways of the lungs begins to swell. Mucus is secreted and the muscles that surround the airway shorten and tighten. These three processes all narrow the airways making it more difficult to breathe. Reliever medications help to reverse this process.
Asthma Medications
Asthma medication is usually given by inhalers with a spacer device and can be used at almost any age. Sometimes inhalers are used in combination with oral medication to control symptoms. Inhalers are divided into two main groups: Relievers and Preventers.
Reliever Inhalers
Reliever inhalers, generally blue in colour, are taken immediately when symptoms occur during an acute exacerbation of asthma. They work quickly to relax the muscles around the airways. This enables the airways to open wider and it becomes easier to breathe again. Common relievers include “ventolin” (salbutamol), “Bricanyl” (terbutaline) and “Atrovent” (ipratropium-bromide). During an exacerbation of asthma, a child may need to take their reliever inhaler up to four times a day until their symptoms have resolved. Once their symptoms are controlled they can discontinue their reliever and return to using it on an “as-needed basis” only. Children with exercise triggered asthma may take their reliever medication before playing sport/PE class.
Preventer Inhalers
A) Inhaled Corticosteroids Alone
Preventer inhalers are taken every day even when the child’s symptoms are well controlled. They act to make the airways less “inflamed/sensitive” and less reactive to asthma triggers. This means that when a child is exposed to asthma triggers he/she is less likely to develop symptoms because the airways are less twitchy and raw. Common names of inhaled corticosteroid preventers include “Becotide” (beclomethasone), “Pulmicort” (budesonide), and “Flixotide” (fluticasone). The steroid-based preventers are generally low dose and safe when used under a doctor’s guidance. A child washes out his/her mouth after taking them to prevent the excess from being absorbed through the lining of the mouth and the development of oral thrush (oral candidiasis). They are usually taken in the morning and evening and therefore should not be needed during school hours.
B) Combination inhalers: steroid plus a long-acting reliever
Combination inhalers incorporate both a “long-acting reliever” and an inhaled corticosteroid preventer medication. They are taken twice a day, morning and evening. Common names of combination inhalers include “Symbicort” (budesonide and formoterol) and “Seretide” (fluticasone and salmeterol).
Types of Inhalers
Different types of inhalers exist including metered-dose inhalers (MDI’s/evohaler), Diskus and Turbuhaler devices. The choice of device depends on the child’s age and inhaler technique. Spacer devices are always used together with MDI’s/evohalers in children but no spacer device is needed with the Diskus or Turbuhaler.
Oral medication (tablets)
Some children are prescribed oral medication in addition to inhalers to control asthma symptoms. Groups of oral preventer medications include
- Leukotrine receptor antagonists eg singulair (montelukast) and accolate (zafirlukast)
- Xanthine theophylline eg Slophyllin
These are generally taken outside school hours. Oral steroids are rarely found in the school environment. They give a much higher dose of steroid than inhaled corticosteroids. During an exacerbation, the doctor may prescribe a 5-day (or longer) course of oral steroids to control severe symptoms.
Spacer devices
Spacer devices make metered dose inhalers easier to use and more effective. They enable more of the medication to reach the site of action in the lung. Because of the coordination required, children under ten to twelve years often cannot use the MDI/evohaler properly without spacer devices. Spacer devices will often be found at the school.
Nebulisers
Normally children do not need to use nebulisers at school because the majority of asthmatics have good symptom control using inhalers and spacer devices, plus or minus oral preventor medication.
WHAT TO DO IF A CHILD HAS AN ASTHMA ATTACK
“The Five Minute Rule”
- Ensure the reliever inhaler is taken immediately. This is usually blue and opens up narrowed air passages.
- Sit the child up and loosen tight clothing.
- Stay calm. Attacks may be frightening and it is important to stay calm.
- If no immediate improvement during an attack, continue to take the reliever inhaler every minute for five minutes or until symptoms improve: two puffs if MDI/evohaler or one puff if turbohaler.
- If symptoms do not improve in five minutes, or if you are in doubt, call 999 or a doctor urgently. Continue to give reliever inhaler.
Asthma in PE and school sports
Full participation in PE and school sports should be the goal for all but the most severely affected children with asthma. However, many children have “exercise triggered asthma” and experience asthma symptoms during exercise. Teachers taking PE class have an important role in supporting and encouraging pupils with asthma. They should:
- Ensure they know which children in the class have asthma.
- Be encouraging and supportive to pupils with asthma.
- Remind children with exercise-induced asthma that some may need to take their reliever ten to fifteen minutes before the start of PE.
- Ensure children bring their reliever inhalers (generally blue) to the gym, sports field or swimming pool.
- Ensure that children who feel they need their asthma medication take their reliever and rest until they feel better.
- Speak to parents if they are concerned a child has undiagnosed asthma.
- Speak to parents or GP to allay any concerns or fears about a child with asthma participating in PE.
What to do when a child with asthma joins your class
If your school has an asthma guideline, ensure you are familiar with it, otherwise take the following steps:
- Enquire from parents about their child’s asthma control and current treatment. This information can be recorded on a school asthma record sheet.
- Allow the child free access to their reliever medication: older children should be allowed to carry their relievers in their pocket and in the case of younger children the reliever should be kept in the classroom in an easily accessible location. Relievers should never be locked away.
- Before exercise, remind the child to carry his/her medication. They may be shy about this, encourage positive attitudes towards pupils with medical conditions.
- On school trips encourage the child to carry his/her medication at all times. Include this information on school circulars to parents.
- Inform the child’s parents if the child has an asthma exacerbation or uses their reliever medication.
- If concerned about a child with “severe symptoms” e.g. missing school or tired in class secondary to disturbed sleep from coughing, speak with parents. Some children with severe asthma may require extra support due to days lost.
How to develop good school asthma management guidelines
The main principles of school asthma management guidelines should:
- Recognise that asthma is an important condition affecting many school children and welcome all pupils with asthma.
- Ensure that children with asthma participate fully in all aspects of school life including PE and sports.
- Recognise that immediate access to reliever inhalers is vital.
- Ensure records of children with asthma and the medication they take are kept.
- Ensure the school environment is favourable to children with asthma.
- Outline what to do in the event of an exacerbation of asthma.
- Work in partnership with all interested parties including school staff, parents, doctors, nurses and children to ensure the school asthma management guidelines are implemented and maintained successfully.
Your Questions Answered
Dealing with medication
Q) Where should the school keep the reliever medication?
Q) What happens if a child takes too much reliever medication?
Q) What if a child without asthma experiments with a reliever inhaler?
Q) Do inhalers go “out of date”?
Q) What happens if a child forgets their reliever inhaler?
Q) Should a child with asthma use another child’s inhaler if they experience asthma symptoms and their reliever (or spare) is not available?
Q) Why is an asthma register important?
Q) How often should the register be updated?
Q) What should happen if a child with asthma is falling behind with lessons because of “missed school days”?
Q) Should asthma be included in the national curriculum or school syllabus?
Q) Do school staff need training?
The legal positions of teachers and school staff.
The Asthma Society of Ireland believes children with asthma should be allowed to take their asthma medication whenever they feel the need. There is no legal or contractual duty on school staff to administer asthma medication or supervise a pupil taking it unless they have been specifically contracted to do so. In emergency situations In an emergency situation e.g. an unexpected acute exacerbation of asthma, school staff are expected to act as any reasonable or prudent parent would. This may include administering medication.
Example of a School Asthma Management Guideline:
A) This school recognises that asthma is an important condition affecting many school age children and positively welcomes all pupils with asthma.
B) This school encourages children with asthma to achieve their full potential in all aspects of school life by having clear guidelines that are understood by staff and pupils.
C) Medication: Immediate access to reliever inhalers is vital.
– Older children are encouraged to carry their reliever inhaler, while reliever inhalers of younger children are kept easily accessible in the classroom
– Parents are asked to ensure that the school is provided with a labeled reliever inhaler and spacer device which the class teacher holds separately in case the child forgets or looses his/hers
– All school staff will let children take their own medication when they need to School staff:Are not expected to administer medication to children except in an emergency, however many of our staff are happy to do this.
D) Record keeping:
- At the beginning of the school year or when a child joins the school, parents are asked if their child has asthma.
- The school asthma record sheet is given to parents of children with asthma and filled out by the child’s GP or asthma nurse.
- School asthma record sheets are sent to parents annually to be updated. If a child’s medication changes parents are asked to inform the school teacher.
E) PE:
- Participation in sport is an important part of school life.
- Children with asthma are encouraged to participate fully in PE.
- Teachers will remind pupils with asthma to complete a warm up of a couple of short sprints over five minutes before the lesson and that some children may need to take their reliever approx. 10 minutes before the start of a PE class.
- Each child’s inhalers are labelled and kept on site at the lesson. Children are encouraged to use their inhaler during PE class if they need it.
F) The school environment:
- The school ensures the school environment is favourable to children with asthma by not keeping furry or feathery pets and having a non-smoking policy. Chemicals in science and art lessons that are potential triggers of asthma are avoided as far as possible.
G) Making the school “asthma friendly”:
- Incorporate asthma into the curriculum: The school ensures that all pupils understand asthma. Asthma can be included in science, geography, history and PE class.
H) When a child is falling behind in lessons:
- If a child is missing lots of school days or is tired in class secondary to disturbed sleep from coughing, the class teacher will talk with parents. Some children may have special educational needs because of asthma. Their medication may need to be adjusted by their GP.
I) Asthma attack:
- The school and school staff follow the below procedure which should be clearly displayed in all classrooms in the event of an asthma attack.
“The Five Minute Rule”
- Ensure the reliever inhaler is taken immediately. This is usually blue and opens up narrowed air passages.
- Sit the child up and loosen tight clothing.
- Stay calm. Attacks may be frightening and it is important to stay calm.
- If no immediate improvement during an attack, continue to take the reliever inhaler every minute for five minutes or until symptoms improve: two puffs if MDI/evohaler or one puff if turbohaler.
- If symptoms do not improve in five minutes, or if you are in doubt, call 999 or a doctor urgently. Continue to give reliever inhaler until help arrives or symptoms improve.
Acid Reflux
What the symptoms of acid reflux are
Acid reflux can cause a range of symptoms. Typical symptoms are heartburn, belching and pain on swallowing. Acid reflux may cause other symptoms that you might not associate with your condition. These include asthma, chronic cough, hoarseness, swelling of the throat, sleep disturbances, nausea and vomiting.
The severity of your symptoms does not always indicate how much the surface of your oesophagus has been damaged. Your doctor may with to determine this by performing an oesophageal endoscopy.
What peptic ulcer disease is
In healthy people, there is a balance between mucus protecting the lining of the stomach and intestine, and attack from acid. Peptic ulcers from when there is either too much acid or too little protection. Other factors such as use of non-steroidal anti-inflammatory drugs (NSAIDS) fro pain relief may cause peptic ulcers to form.
Causes of and protectors against peptic ulcer disease
- Attacking factors
- Stomach acid
- Pepsin – a digestive enzyme
- Stomach bacterium Helicobacter pylori
- NSAIDS
Protective factors
- Mucus formation
- Blood supply to the surface of the stomach and intestine (called the mucous membrane)
- Regenerative of the mucous membrane
What the symptoms of peptic ulcer disease are
Typical symptoms of peptic ulcer disease are a pain in the stomach, heartburn, belching, nausea, vomiting, bloating, flatulence and general digestive disorders.
Tips for taking your medicine correctly – To help you remember to take your medicine.
Place a note in a prominent place as a reminder by putting it where you will see it each day, for example, on your bathroom mirror or on your computer at work. Keep your tablets next to something you use at least once a day, for example, next to your alarm clock.
How you can help yourself – watch what you eat and drink
Never eat too much in one go – it is better to eat smear amounts more often. Avoid fatty and spicy foods and also deserts – protein-rich food is better for you. Avoid alcohol and drinks containing caffeine (coffee, tea and cola) as they stimulate acid production in the stomach. Avoid eating immediately before going to bed.
Changes to make to your lifestyle
Slightly raise the head of your bed to avoid lying in a completely flat position. Try to take a gentle walk after eating rather than a snooze. Do not put yourself under unnecessary stress. Try to take things easy and take some time to relax. Try not to smoke.
If you are overweight, losing a few pounds help relieve some of the pressure on your stomach. Wear comfortable, loose-fitting clothing.
If you would like additional information about your condition and its treatment, ask your doctor or pharmacist.
What is COPD?
COPD includes chronic bronchitis, emphysema, or both. Most COPD patients have both.
Millions of people have COPD, both men and women. It is also a leading cause of disability and death. Experts estimate that up to 11 million Americans have COPD. However, just as many people have some form of lung problem but haven’t been diagnosed with COPD.
Do you have breathing problems? Find out how serious they are with this symptom checker.
The most common cause of COPD is smoking. It is 10 times more likely that a smoker will die from it than a nonsmoker. Secondhand tobacco smoke may also increase a person’s chance of getting COPD.
Another cause of COPD is exposure to indoor or outdoor pollutants. It can also be caused by a rare genetic condition called Alpha-1 Antitrypsin Deficiency.
COPD is a progressive condition. But it can be treated.
COPD can cause you to be less and less active over time, which can lead to you becoming more and more out of shape. And that can make it even harder for you to breathe. That’s why it’s so important to manage your COPD.
COPD can affect your life as early as your 40s. But COPD is often underdiagnosed and undertreated. This can be because COPD is often confused with other issues.
The good news is that there are many things you can do to manage your COPD.
Learn how to live with COPD by doing things like exercising regularly, eating healthy foods, quitting smoking, and making other lifestyle changes.
Living with COPD
Your COPD can be managed and treated. But you need to talk to your doctor. Set goals with him or her about the lifestyle changes you should make. For example, you could start exercising more and go on a prescription treatment to better manage your condition.
Ask your doctor if a prescription treatment is right for you. Talk about the two types of therapy for people with COPD: long-term, daily maintenance and rescue medicines. They may help with your breathing problems. Your doctor may prescribe one or both types; it depends on your health and symptoms. Some patients are on more than one maintenance medicine.
There are many prescriptions available, both daily maintenance and rescue, for the treatment of COPD.
Click here to learn more about one prescription maintenance treatment option.
In addition to prescription options, you can also take actions that may lead to a better life. Start now by taking a few small steps in the right direction. It may lead you down a path of healthy living.
What is an Allergy?

Allergens
An allergen is a general term used to describe something that causes an allergic reaction. Allergens are actually tiny proteins found on certain substances. Some examples are airborne allergens, like pollen and mould; foods like shellfish, peanuts and milk. Venom from an insect sting contains allergens as do plants, like poison ivy. Allergens also exist in households, like dust mites. Only those who are prone to acquired sensitivity are regularly affected by these allergens.
Pathway of an Allergic Reaction
Two phases exist in allergic reactions, primary exposure and re-exposure. In this example, the primary exposure is from allergens in the venom of an insect sting.
Anaphylaxis: An Allergic Emergency
Anaphylaxis is a life-threatening reaction. The onset of this reaction occurs within seconds or minutes of exposure. Symptoms include red raised blotches over most of the body, skin becomes warm to the touch, intense tightening and swelling of the airway make breathing difficult, and there is a drop in blood pressure. Breathing can stop and the body may slip into shock. If medication is not quickly administered, heart failure and death can result within minutes. Allergens in insect venom and injectable medications are more likely to cause anaphylaxis than any other allergen. Anaphylaxis is not a common reaction and can be controlled with prompt medication and the help of a physician.
The Immune System
The immune system consists of two types of white blood cells called T-cells and B-cells. These cells help the immune system defend our body by recognizing foreign and potentially harmful substances and then releasing potent chemicals to combat the foreign invader. An allergic reaction occurs when the immune system mistakenly recognizes a harmless substance (such as pollen) and becomes sensitive to that substance. Repeated exposures to the substance, even years later, can trigger an allergic reaction.
Who gets Allergies?
The tendency to develop allergies is thought to be inherited because they commonly develop in those who have a family history. However, it is possible for anyone to develop allergies at any age. Environmental factors can make our immune systems overly sensitive. This could then trigger allergies in people with no family history or help its onset in those that have a family history.
Primary Exposure
T-cells recognize the foreign allergen and release chemicals, which instruct B-cells to produce millions of antibodies, called IgE. (Each time a different type of allergen triggers IgE production, a new type of IgE is produced, specific to that allergen). IgE’s then attach themselves to mast cells. Mast cells with attached IgE’s can remain in the body for years, ready to react with the same allergen.
Re-exposure
With re-exposure, allergens re-enter the body and directly contact the IgE antibodies attached to the mast cells. This stimulates the mast cells to quickly release chemicals like histamine. The release of these chemicals can cause tightening of smooth muscles in the airways; dilating small blood vessels and making them leak (resulting in warming and swelling of skin tissues); increasing mucus secretion in nasal cavity and airways; and itching.
Causes of Allergies
About 40% of us suffer from some form of allergies. And they’re particularly bad during spring and fall when pollens and moulds are high.
But allergies aren’t just about a runny nose and scratchy throat. In fact, allergies are caused by a reaction in your immune system.
- Anaphylaxis
- Chemical Allergy
- Seasonal Rhinitis (Hay Fever)
- Allergy to Household Dust
- Non-seasonal Rhinitis
- Allergic Asthma
- Allergy to Animals
- Allergies to Insect Stings
- Skin Allergies
- Eczemas
- Food Allergies
- Food Sensitivity
- Allergies to Medicine
Allergy Diagnosis
Everyone is individually unique. Allergy tests provide concrete specific information about what you are and are not allergic to. You or your attending physician need not to guess inaccurately any longer. Be certain. No more guessing!
Skin Testing for allergy
There are various methods of allergy testing. The simplest of which is skin prick testing or intradermal testing. Although slightly cheaper, these tests cannot be carried out on patients who are on many common medications, may not be as accurate unless done properly by highly trained personnel, may cause minor pain and discomfort with multiple needles being utilized and most importantly although rare, carry an increased risk of severe side effects such as anaphylaxis. The number of substances being tested is also very limited. This is still a good but basic testing modality.
In-Vitro Testing
Assessing the level of allergen-specific IgE in a patient’s serum in conjunction with a clinical evaluation based on patient history and subsequent testing can help a doctor confirm a diagnosis of atopic allergy and assist in the treatment of the patient.
Treatment Options
Once a diagnosis of atopic allergy to one or more specific substances is made, doctors have several treatment options to consider:
- Have patients avoid subsequent exposure to identified allergen(s)
- Employ a course of state of the art pharmacotherapy to treat allergic symptoms
Immunotherapy
Desensitize patient with Immunotherapy that employs controlled, prolonged exposure to specifically identified allergens. Sublingual Allergen Immunotherapy (SLIT) and Specific (Injectable Subcutaneous) Immunotherapy (SIT) is a highly effective treatment for carefully selected patients who have an allergy to cat/dog/horses and allergic rhinitis due to house dust mites, grass pollens, certain tree pollens and certain weed pollens. It is effective in selected asthmatics but is not effective for food allergies or eczema.
The course of treatment is for 3 years and this confers immunity to the specific allergen for up to 10 years and also decreases the onset of new allergies for many years after.
In any case, the success of treatment depends upon accurate identification of the offending allergen(s) and a knowledge of the patient to subsequent allergen exposure.
Managing Allergies
The first step to managing allergies is to identify what type of reaction you’re having, whether it is watery eyes, sneezing or difficulty breathing.
Secondly, try to identify the trigger or the situation, which led to the symptoms. Ask a few questions:
- Where did the reaction occur?
- Inside or outside?
- Were you eating or drinking?
- Were there any animals or insects near you?
- Were you wearing something new?
- Or did you use a new soap or detergent?
A physician can do an allergy test with a variety of common allergens to determine your allergy. Once the allergen has been identified, manage your allergies by following some simple tips:
- Avoid allergens
- Avoid tobacco smoke or other irritants
- Use medication as prescribed
- See a doctor regularly
- Stay healthy
A clear understanding of the disease and social support in living with it are very important for the success of asthma therapy. In many countries, associations exist to ensure that asthma sufferers are never alone in their daily battle. Their activities include educational meetings, summer and winter camps to help asthmatics learn how to control their disease whilst engaging in physical activity (e.g. walking, hiking, gymnastics, swimming, canoeing), telephone helplines, etc.
Ask your doctor for the name and address of the association in your area. And take full advantage of the services they offer!
Asthmatics themselves can have considerable control over how often they suffer an attack and how rapidly they recover. It all depends on taking some precautions.
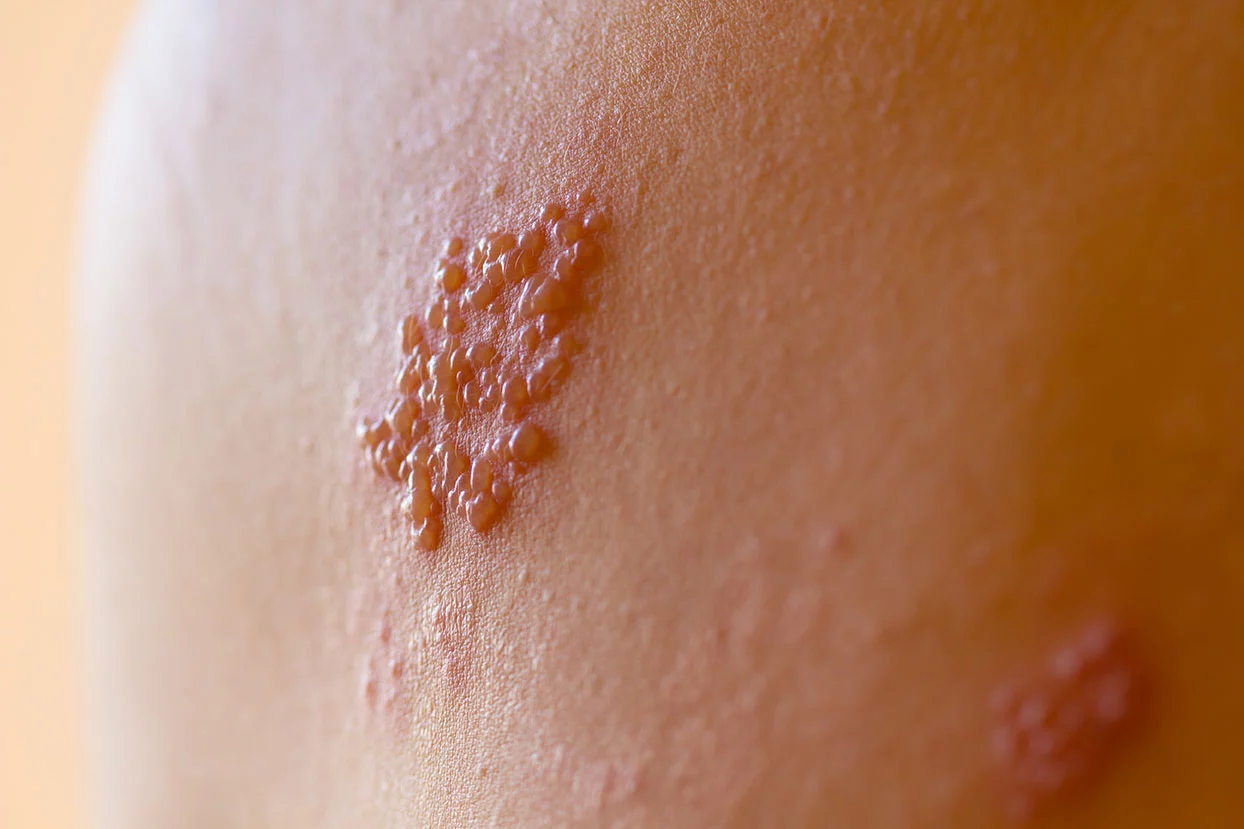
The Facts About Shingles
As a child, you may remember coping with chickenpox – an itchy rash consisting of blisters. Now you have those blisters again, but instead of itching, they are painful. Are you experiencing another outbreak of chickenpox? Maybe not—you may be experiencing an outbreak of shingles.
Shingles is an infection caused by a reactivation of the varicella-zoster virus, the same virus that causes chickenpox. After the chickenpox blisters have healed, the varicella-zoster virus lies dormant (inactive) in neurons (nerve cells) next to your spinal cord, sometimes for decades. When the virus becomes active again, it travels down the nerve fibres that extend to your skin, and a rash develops. The main difference between chickenpox and shingles is that shingles generally erupts in a band (dermatome) on one side of the body, rather than all over your body.
Many people who develop shingles find that pain is the most difficult aspect of this condition to deal with. For some people, the aftereffects of shingles can last longer than the rash. Postherpetic neuralgia (PHN) is a painful complication of shingles caused when the infection damages the nerves.
Who Gets Shingles?
Shingles is an infection caused by the varicella-zoster virus, the same infection that causes chickenpox. The main difference, however, is that shingles generally erupts in a band on one side of the body, rather than all over your body.
After the chickenpox blisters have healed, the varicella-zoster virus lies dormant (inactive) in neurons (nerve cells) next to your spinal cord, sometimes for decades. When the virus becomes active again, it travels down the nerve fibres that extend to your skin, and a rash develops.
Who Is at Risk?
Anyone who has had chickenpox is at risk of developing shingles. Young people can get shingles, this disease usually occurs in people over age 50. The frequency of shingles is basically constant between the ages of 20 and 50 years (2.5 cases per 1,000 people per year). The chances of getting shingles then double in people between ages 50 and 60 years and then doubles again in people age 80 to 90 years.
An important factor, though, is the immune system, which helps keep viruses at bay. The varicella-zoster virus can become active again because of a decrease in a person’s immunity to the virus. This decrease in immunity can occur with advanced age. However, sometimes it is not known why the virus becomes active again.
The following may cause the varicella-zoster virus to become active and cause an outbreak of shingles:
- Diseases that affect the immune system (eg, non-Hodgkin’s lymphoma and HIV)
- Anticancer and immunosuppression drugs that suppress the immune system (eg, chemotherapy)
- Temporary depression of the immune system from a cold or sunburn
- Stress (due to negative life events)
- Major depression
Shingles in Children
Children whose mothers developed chickenpox within 5 to 21 days before giving birth are susceptible to developing shingles. These babies are usually born with chickenpox or develop it within a few days of birth. One-third of these children develop shingles during the first 5 years of their life.
Can I Get Shingles Again?
Most people who get shingles develop immunity to the varicella-zoster virus and will not get it again. Only about 4% of people will have another outbreak in the future. When shingles do recur, it is often in people with a compromised immune system (eg, they are infected with HIV or are undergoing chemotherapy treatments). A second outbreak of shingles may occur many years after the first outbreak. When shingles do recur, the rash usually does not appear in the same location as the first outbreak.
Can I Catch Shingles?
You cannot catch shingles from someone who has it. However, the rash that occurs with shingles sheds the same varicella-zoster virus that causes chickenpox and may be contagious. So, if you have not had chickenpox or have not been vaccinated against the varicella-zoster virus, you can develop chickenpox (not shingles) if you come in contact with someone who has shingles. People with shingles can transmit the virus only if the blisters have broken and the virus is transmitted when skin-to-skin contact with broken blisters occurs.
Some people with shingles may feel quite ill at first, almost as though they have the flu. These symptoms—fever, headache, nausea, and chills—may be part of the prodromal stage (prodrome refers to symptoms that appear before the rash appears).
Shingles occur in two stages—the prodromal stage and the eruptive stage.
Prodromal Stage
The prodromal stage occurs about 2 to 5 days before the rash appears. Symptoms during the prodromal stage may include:
- Fever, headache, nausea, and chills
- Numbness on one side of the body or face
- Tingling, burning, or shooting pain on one side of the body or face (pain may be constant or intermittent)
- Itching on one side of the body or face
Eruptive Stage
During the eruptive stage, redness and swelling will appear at the site of the pain, along with clusters of blisters filled with clear fluid. New blisters will continue to appear for up to 5 days. These blisters can be scattered in patches or form a continuous band on the skin (dermatome), and they look a lot like chickenpox. The blisters can be mildly irritating, itchy, or intensely painful. Within 14 days, the blisters become filled with pus and then form a scab. At this point, they no longer contain the virus. The rash usually goes away in about 3 to 5 weeks. The blisters leave no scars, but you may have discolouration of the skin where they once were.
Symptoms
The rash and blisters from shingles almost always occurs on just one side of the body. Shingles may appear on the following areas of the body:
- One side of the torso
- Waistline
- One side of the face
- Buttocks
- Arm
- Leg
The pain associated with shingles has been described as intense and sometimes unrelenting. If you think you are experiencing symptoms of shingles, it is very important that you see your doctor right away.
Without treatment, the symptoms of shingles (eg, rash, blisters, and pain) usually go away in about 3 to 5 weeks. Although shingles can make you very uncomfortable while you have it, it usually is not dangerous to healthy people. However, some people may develop complications from shingles, such as continued severe pain after the blisters are gone. This condition is called postherpetic neuralgia (PHN), and can be extremely painful and very hard to cope with. The pain from PHN may last for months and even years.
Shingles Complications
In healthy people, the rash, blisters, and pain of shingles usually go away in about 3 to 5 weeks. Although shingles can make you very uncomfortable while you have it, it usually is not dangerous to healthy people. But in people with a weakened immune system, shingles can be life-threatening. You should see your doctor immediately if you think you may have any complications of shingles. He or she can help provide treatment and watch your progress.
Postherpetic Neuralgia (PHN)
PHN is the most common complication of shingles. It is a condition in which severe pain from shingles may last for months, and sometimes years after the shingles rash has healed. PHN occurs from damage to the nerve fibres, caused by the varicella-zoster virus. Nerve fibres send messages from the skin to the brain. When nerve fibres are damaged during an outbreak of shingles, they are not able to send messages as they normally do. The body may perceive these “mixed messages” as pain.
Hutchinson’s Sign*
Hutchinson’s sign occurs when a shingles blister(s) appears on the tip of the nose. It indicates that the herpes zoster virus has invaded the nerve in the eye (ophthalmic nerve), and will cause painful swelling of the eye. This inflammation can cause temporary blindness and vision loss. You should see an eye specialist (ophthalmologist) immediately if you have shingles blisters on the tip of your nose.
Ramsay Hunt Syndrome*
The Ramsay Hunt Syndrome occurs when the herpes zoster virus spreads to the facial nerve, which causes intense ear pain. The shingles rash may appear on the outside of the ear, inside the ear canal, around the mouth, on the roof of the mouth, and on the neck, face, and scalp. When the shingles virus affects the facial nerve, hearing loss, dizziness, and facial paralysis may occur, which is usually temporary, but not always. If you experience shingles blisters on your ear, mouth, neck, face, or scalp, see your doctor right away.
Bacterial Skin Infection
The shingles rash may be itchy. Scratching the rash may damage the skin and introduce bacteria from the fingernails, resulting in a bacterial infection. A shingles rash that does not heal may be an indication that a bacterial infection is present. See your doctor immediately if the rash has worsened or is not healing.
Infection of Internal Organs
Your immune system, which protects your body from infections and disease, can become weakened from certain diseases and treatments. HIV infection and cancer are two diseases that weaken a person’s immune system. People who have received an organ transplant take drugs that suppress their immune system so their body will not reject the transplant. Treatment for cancer may also weaken the immune system because it can damage cells of the immune system along with destroying cancerous cells.
Shingles can be dangerous in someone with a weakened immune system because the zoster virus can possibly spread throughout the body and reach vital organs like the lungs, central nervous system, and brain. A widespread infection like this can cause viral pneumonia or a secondary bacterial infection, which can be life-threatening. If you believe that you have a weakened immune system and develop shingles, it’s important to see your doctor immediately.
What Causes Arthritis?
- Genetics
- Lifestyle
- Autoimmune disorders
- Environment
Do you suspect you have arthritis?
Your doctor is the best person to diagnose if you have arthritis. His or her diagnosis can be based on:
- A detailed medical history of current and past symptoms
- A physical examination
- X-rays
- Blood work
Additional healthcare providers who help manage arthritis. Your doctor may refer you to:
- Rheumatologists
- Physical therapists
- Occupational therapists
- Surgeons
You’ve probably heard the word “arthritis” before. And now, you may be wondering if it could be affecting you. By definition, arthritis means “joint inflammation,” and it’s used to describe more than 100 different diseases and conditions that affect joints, the tissues that surround joints, and other connective tissue.
Arthritis can affect people differently. It’s common in adults 65 and older, but it can affect people of all ages, races, and ethnic groups. In fact, 1 out of every 5 adults in the United States — over 46 million people — has reported being diagnosed by their doctor with some form of arthritis.
Two of the most common forms of arthritis are osteoarthritis and rheumatoid arthritis.
Osteoarthritis and rheumatoid arthritis have different causes, risk factors, and effects on the body:
- Osteoarthritis pain, stiffness, or inflammation most frequently appears in the hips, knees, and hands.
- Rheumatoid arthritis commonly affects the hands and wrists but can also affect areas of the body other than the joints.
Even though they have these differences, osteoarthritis and rheumatoid arthritis often share common symptoms:
- Joint pain
- Stiffness
- Inflammation or swelling
The importance of talking to your doctor
Sometimes arthritis symptoms make it harder to do certain activities. By talking to your doctor about your symptoms, he or she may help you find other ways to continue doing some of those activities.
Your doctor can also help evaluate your current treatment and may recommend other, more effective ways to help you manage your arthritis. The sooner you take action and talk to your doctor, the sooner you can start managing your arthritis symptoms more effectively.
Treatment
Get the conversation started. Part of taking an active role in managing your arthritis is knowing what your treatment options are. An informed decision made with your doctor can be one of the best decisions you can make to help you get effective symptom relief.
It’s important to understand that although there is no way to reverse the cartilage loss of osteoarthritis or rheumatoid arthritis, there are treatment options available to help you relieve the symptoms. These can include:
- Medications
- Exercise
- Diet
- Alternative therapies
- Surgery
Your doctor may even suggest combining several treatment options to more effectively manage your arthritis symptoms. Every situation is different, so discuss your symptoms and your lifestyle with your doctor so you can work together for the best option or options for you.
Medication can help you manage arthritis symptoms, but there are other things you can do in addition to medication.
There are other things you can do to help manage your arthritis symptoms:
Medications are an important part of managing arthritis symptoms. But medication alone may not be enough. Guidelines from both the American College of Rheumatology (ACR) and the Osteoarthritis Research Society International (OARSI) suggest taking an active approach that includes medication as well as lifestyle changes to more effectively manage arthritis symptoms.
Keep Fit
- Follow a healthy diet.
- Find a balance between physical activities (like walking or water aerobics) and rest.
Keep Informed
- Don’t be afraid to ask your doctor questions about arthritis or your treatment.
- Use books, magazines, and online resources to learn more about arthritis and stay up to date on new developments in medicine and treatment options.
Keep Working with Your Doctor
- Talk to your doctor about changes in your arthritis symptoms to help him or her determine the right treatment for you.
- Always take your medication as your doctor prescribes.
- Be sure to report any changes in your health or any side effects that you may experience. Your doctor needs that information to make sure that your treatment is the right one for you.
Being overweight increases the risk of developing OA. Even a little weight loss can make a difference when it comes to reducing stress on your joints, especially the knees. For every pound you lose, you remove about 4 pounds of stress from your knees.
The Role of Nutrition
Along with regular exercise, a balanced diet is important in helping you lose weight. Here are a few nutritional tips:
- Eat a variety of foods, focusing on a greater proportion of whole grain products, vegetables, and fruit.
- Keep your diet low in fat, saturated fat, and cholesterol — and moderate in sugars.
- Choose foods that are rich in polyunsaturated fatty acids and antioxidants. Fish such as salmon, lake trout, and albacore tuna, as well as fish oil, contain high amounts of omega-3 fatty acids.
- If you drink alcohol, do so in moderation.
Migraine
Headache / Migraine
A migraine is a common type of headache that may occur with symptoms such as nausea, vomiting, or sensitivity to light. In many people, a throbbing pain is felt only on one side of the head.
Some people who get migraines have warning symptoms, called an aura, before the actual headache begins. An aura is a group of symptoms, including vision disturbances that are a warning sign that a bad headache is coming.
Causes, Incidence, and Risk Factors
Migraine headaches tend to first appear between the ages of 10 and 45. Sometimes they may begin later in life.
- Migraines occur more often in women than men.
- Migraines may run in families.
- Some women, but not all, may have fewer migraines when they are pregnant.
A migraine is caused by abnormal brain activity, which is triggered by stress, certain foods, environmental factors, or something else. However, the exact chain of events remains unclear. Today, most medical experts believe the attack begins in the brain and involves various nerve pathways and chemicals. The changes affect blood flow in the brain and surrounding tissues.
Migraine attacks may be triggered by:
- Alcohol
- Allergic reactions
- Bright lights
- Certain odours or perfumes
- Changes in hormone levels (which can occur during a woman’s menstrual cycle or with the use of birth control pills).
- Changes in sleep patterns
- Exercise
- Loud noises
- Missed meals
- Physical or emotional stress
- Smoking or exposure to smoke
Symptoms
Vision disturbances, or aura, are considered a “warning sign” that a migraine is coming. The aura occurs in both eyes and may involve any or all of the following:
- A temporary blind spot
- Blurred vision
- Eye pain
- Seeing stars or zigzag lines
- Tunnel vision
Not every person with migraines has an aura. Those who do, usually develop one about 10 – 15 minutes before the headache. However, it may occur just a few minutes to 24 hours beforehand. A headache may not always follow an aura.
Migraine headaches can be dull or severe. The pain may be felt behind the eye or in the back of the head and neck. For many patients, the headaches start on the same side each time. The headaches usually:
- Feel throbbing, pounding, or pulsating
- Are worse on one side of the head
- Start as a dull ache and get worse within minutes to hours
- Last 6 to 48 hours
Other symptoms that may occur with the headache include:
- Chills
- Increased urination
- Fatigue
- Loss of appetite
- Nausea and vomiting
- Numbness, tingling, or weakness
- Problems concentrating, trouble finding words
- Sensitivity to light or sound
- Sweating
Symptoms may linger even after the migraine has gone away. Patients with migraine sometimes call this a migraine “hangover.” Symptoms can include:
- Feeling mentally dull, like your thinking is not clear or sharp
- Increased need for sleep
- Neck pain
Signs and tests
Your doctor can diagnose this type of headache by asking questions about your symptoms and family history of migraines. A complete physical exam will be done to determine if your headaches are due to muscle tension, sinus problems, or a serious brain disorder.
There is no specific test to prove that your headache is actually a migraine. However, your doctor may order a brain MRI or CT scan if you have never had one before or if you have unusual symptoms with your migraine, including weakness, memory problems, or loss of alertness.
An EEG may be needed to rule out seizures. A lumbar puncture (spinal tap) might be done.
Treatment
There is no specific cure for migraine headaches. The goal is to prevent symptoms by avoiding or changing your triggers.
Treatment is naturally an individual matter. Some people have infrequent mild episodes, requiring a little peace and quiet while others have disabling attacks every few weeks, needing preventive daily therapy to suppress them.
A good way to identify triggers is to keep a headache diary. Write down:
- When your headaches occur
- How severe they are
- What you’ve eaten
- How much sleep you had
- Other symptoms
- Other possible factors (women should note where they are in their menstrual cycle)
For example, the diary may reveal that your headaches tend to occur more often on days when you wake up earlier than usual. Changing your sleep schedule may result in fewer migraine attacks.
When you do get migraine symptoms, try to treat them right away. The headache may be less severe. When migraine symptoms begin:
- Drink water to avoid dehydration, especially if you have vomited
- Rest in a quiet, darkened room
- Place a cool cloth on your head
Many different medications are available for people with migraines. Medicines are used to:
- Reduce the number of attacks
- Stop the migraine once early symptoms occur
- Treat the pain and other symptoms
Expectations (Prognosis)
Every person responds differently to treatment. Some people have rare headaches that require little to no treatment. Others require the use of several medications or even occasional hospitalization.
Complications
Migraine headache is a risk factor for stroke in both men and women.
Migraine headaches generally represent no significant threat to your overall health. However, they can be a long-term (chronic) problem and may interfere with your day-to-day life.
See your doctor if:
- You are experiencing “the worst headache of your life”.
- You have speech, vision, or movement problems or loss of balance, especially if you have not had these symptoms with a migraine before.
- Your headaches are more severe when lying down.
- The headache starts very suddenly.
Prevention
Understanding your headache triggers can help you avoid foods and situations that cause your migraines. Keep a headache diary to help identify the source or trigger of your symptoms. Then modify your environment or habits to avoid future headaches.
Other tips for preventing migraines include:
- Avoid smoking
- Avoid alcohol
- Avoid artificial sweeteners and other known food-related triggers
- Get regular exercise
- Get plenty of sleep each night
- Learn to relax and reduce stress — some patients have found that biofeedback and self-hypnosis helps reduce the number of migraine attacks
For more information or to book an appointment, contact us today on (01) 873 59 59.
Self Treatment of Common Illnesses and Accidents
Burns
Apply large quantities of cold water to the affected area as soon as possible and maintain this until the pain subsides. This may take as long as 15minutes!. If the skin is unbroken but blistered, apply a loose dry dressing. If the burn is larger that 4 or 5 inches in diameter or if the skin is broken, consult your doctor as soon as possible.
Colds
Even in this day and age there is still no magic cure for the common cold. Go to bed, take plenty of drinks. If you have a headache or are feverish, take aspirin or paracetamol. Do not bother to take any antibiotics you may have in the house – these will have no effect!
Sprains
Firstly apply a cold compress, containing ice if possible, for 15 to 30minutes to reduce the swelling. Apply, firmly a crepe bandage and give the sprain plenty of rest until all discomfort has subsided. Further strain will inevitably lead to further swelling and a longer recovery period.
Nose Bleeds
Sit in a chair (leaning forward with your mouth open) and pinch your nose just below the bone for approximately 10 minutes, by which time the bleeding should have stopped. Avoid hot drinks or food from 24hrs. If symptoms persist, consult your doctor.
Minor cuts & Grazes
To stop the bleeding apply a clean handkerchief or dressing firmly for about 5 minutes. Cover with a clean dry dressing.
Sunburn
Treat as for other burns with cold water to remove the heat. Calamine lotion will relieve the irritation whilst paracetamol will also help. Children are particularly susceptible to sunburn and great care should be taken to avoid over-exposure to the harmful effects of the sun.
Insect bites & stings
Antihistamine tablets can be obtained from the chemist without prescription and will usually relieve most symptoms. Note: bee stings should be scraped away rather that plucked in order to avoid squeezing the contents of the venom sac into the wound.
Chickenpox
The rash appears as small patches or blisters. During the next 3 or 4 days, further patches will appear and the earlier ones will turn ‘crusty’ and fall off. Oily calamine lotion may be applied to soothe the often severe itching. Cool baths may also help. It is infectious a few days before the rash appears until all the lesions have scabbed. Children may return to school as soon as the last ‘crusts’ have dropped off.
Measles
The rash is blotchy and red and appears on the face and body on the first day of illness. It is infectious a few days before the rash appears until 5 days after. Immunisation can prevent this disease.
Mumps
Symptoms are swelling of the glands in front of one of the ears often followed after a couple of days by swelling in front of the other ear. It is infectious 7 days before the swelling appears until 9 days after that date. If the pain is severe you should consult your doctor. Immunisation can prevent this disease.
Earache
Most earache occurs in children and a majority of infections will settle without antibiotics. If your child develops earache we recommend paracetamol and fluids, until arrangements can be made to see a doctor. Your child should be seen if the symptoms persist for more than one or two days or if symptoms are severe.
Sore throat
The great majority of sore throats settle with the same treatment as for colds and flu. We would only normally consider using antibiotics if a sore throat has persisted for more than a week or was especially severe.
Diarrhoea and vomiting
In adults and older children, diarrhoea and vomiting will usually get better on its own. Treatment consists of replacing the fluid you have lost and resting the digestive system by having nothing solid to eat for 24 hours. Sachets of powder such as Dioralyte and Rehidrat which can be made up into a drink are available from the chemist. Dairy products are best avoided for a few days. If the diarrhoea contains blood or there is severe pain or high fever, you should discuss your symptoms with a doctor. Diarrhoea and vomiting in small babies and young children should be treated with caution.
High blood pressure
Everyone has blood pressure. It shows the amount of work that your heart has to do to pump blood around the body. Blood pressure is the pressure that blood exerts against the inner walls of blood vessels as it is pumped through the circulatory system. Blood pressure levels are represented by two numbers. Normally a healthy person has arteries that are strong, flexible and muscular. When the heart contracts, the force of blood against artery walls increases. This force or pressure is called systolic pressure, and it is the number at the top of a blood pressure reading. When the heart relaxes it causes the pressure against artery walls to decrease. This second pressure is called diastolic pressure and is the number at the bottom of a blood pressure reading.
Anyone can have high blood pressure, but certain risk factors can raise your blood pressure. These factors include family history, gender, increasing age, being overweight, high intake of salt in the diet and ethnic origin. Other factors include high intake of alcohol, smoking, lack of exercise and use of certain oral contraceptives.
High blood pressure is a ‘silent’ disease. A person with high blood pressure may feel well, look well and may rarely have any symptoms. High blood pressure can cause damage over the years which may lead to a heart attack or stroke at an earlier age than people with normal blood pressure. Your doctor can explain this to you in greater detail. Although high blood pressure cannot be cured, it can be controlled with diet, exercise, and lifestyle changes with or without medication.
How can I reduce my blood pressure?
- Stop smoking
- Drink alcohol in moderation
- Increase your intake of fruit and vegetables
- Exercise regularly
- Maintain healthy weight
- Take your hypertension medicine as directed by your doctor